CaseManager
iPad and iPhone app to enable insurance company Case Managers to better engage with members in order to lower hospital readmissions.

iPad and iPhone app to enable insurance company Case Managers to better engage with members in order to lower hospital readmissions.


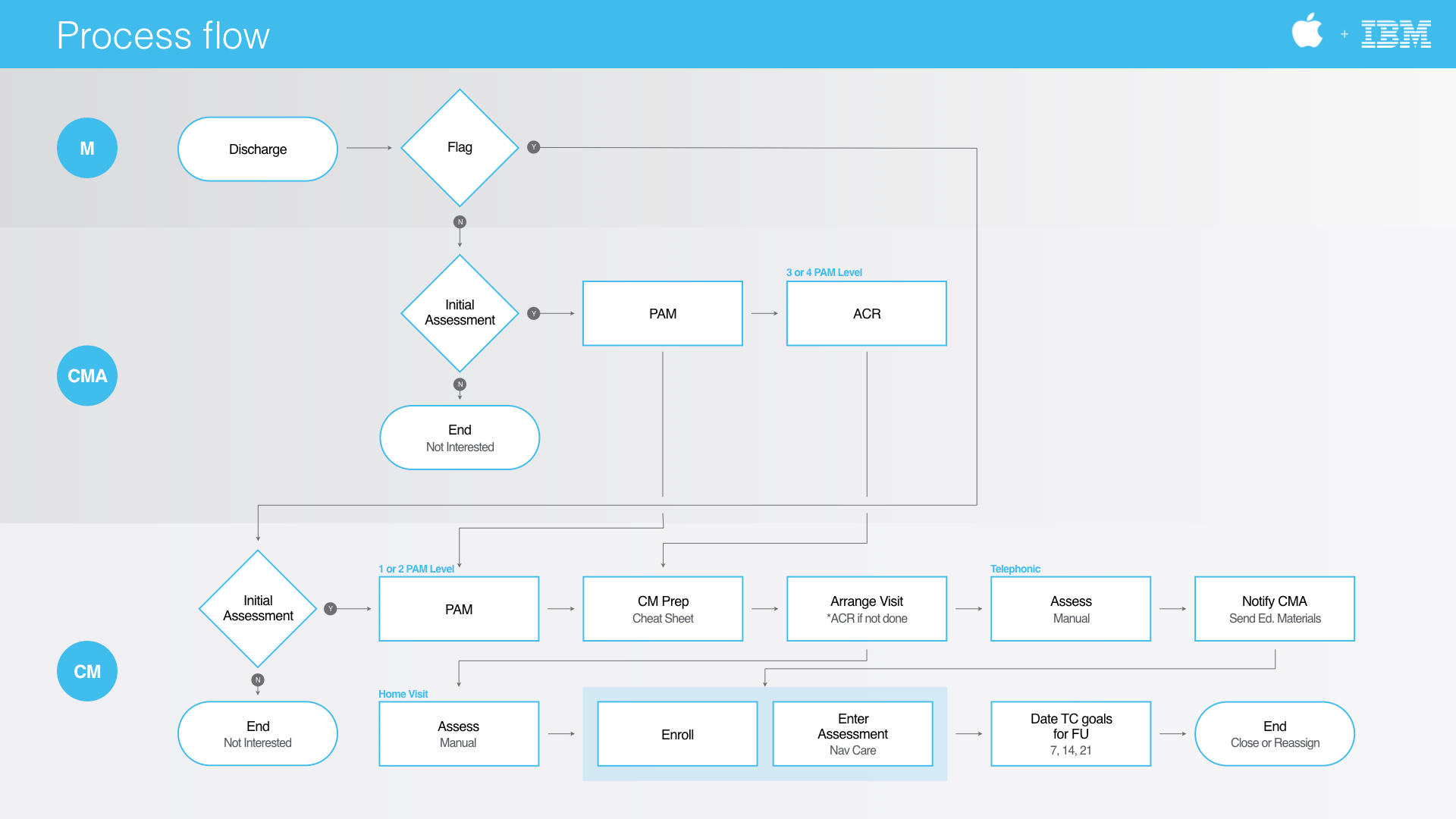
Case Managers have a challenging job whose primary goal is to reduce hospital readmissions by following up with patients to check on wellbeing and encourage adherence to their discharge orders. They represent insurance companies, but are often were previously nurses and can often have to walk an uncomfortable line between checking in on member and giving care. Additionally, CM's largely work remote, but still have to juggle the complexities of a paper-based workflow while maintaining HIPAA compliance

Three areas of focus drove the design of the app. We aimed to make it easy to plan for the day, remove the confusion navigating HIPAA, enable CM's to be able to do more in home assessments.
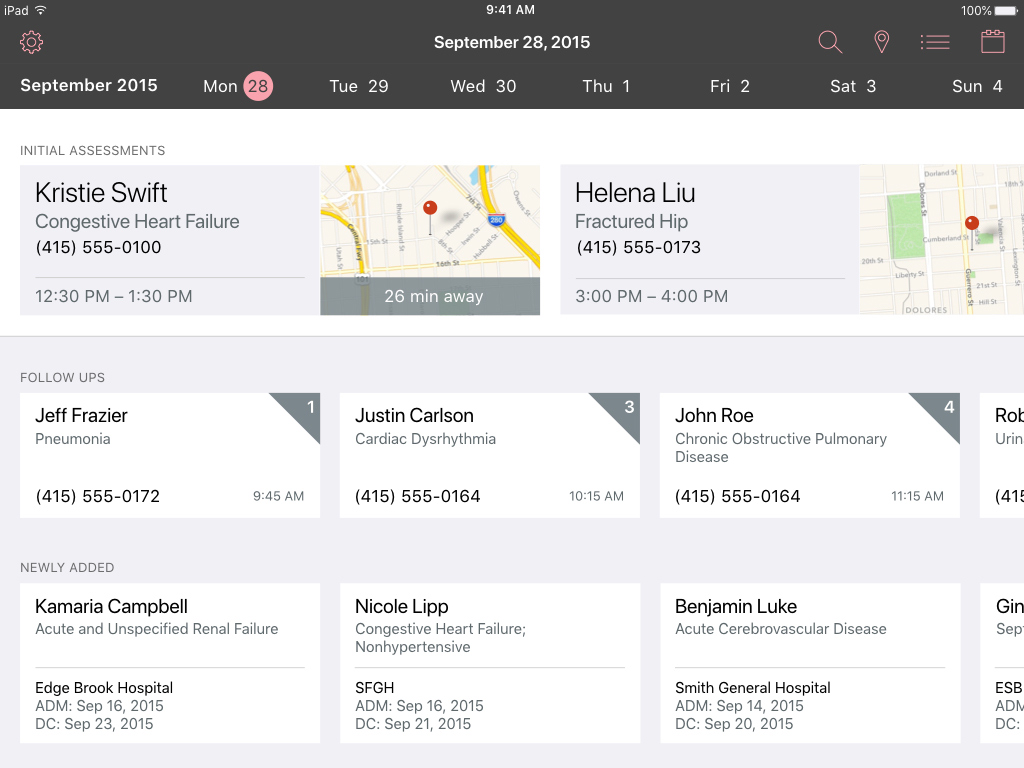
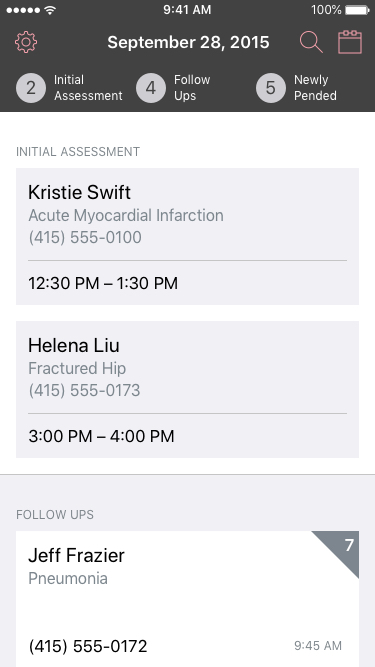
Every day for a CM is different, often their schedule is managed by their CMA's Understanding what the days responsibilities are so the can prepare for every conversation was a challenge. The hierarchy driven card rows give context, while calendar and map views help them prioritize.




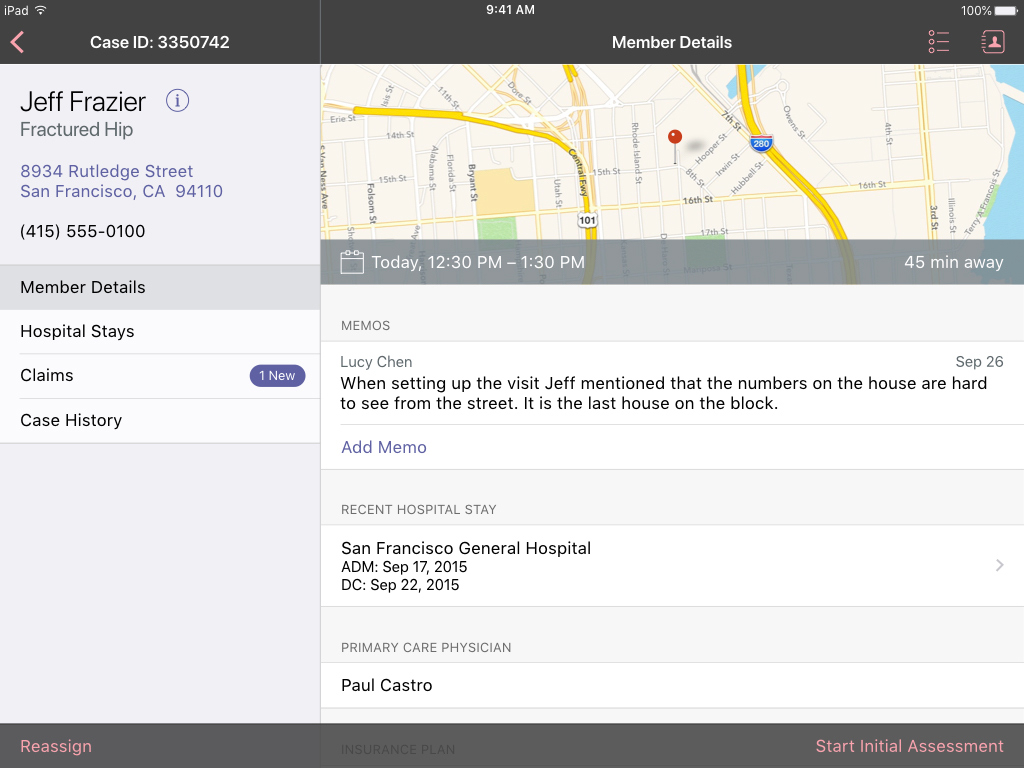
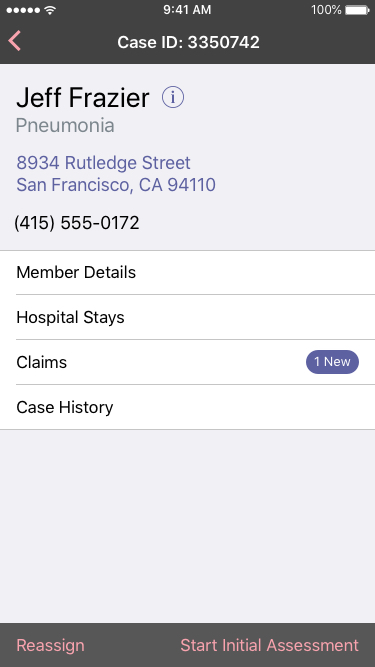
Remote CM's encumbered by HIPAA complexities meant they didn't always have up to date case or member details unless they traveled to pick up physical records. The app managed document compliance, and assured the most up-to-date records and notes from the whole care team.



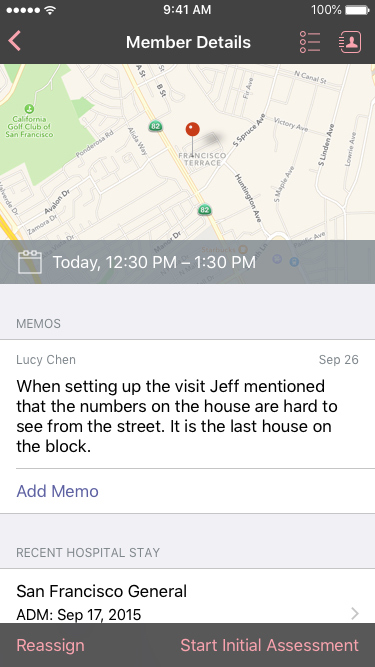
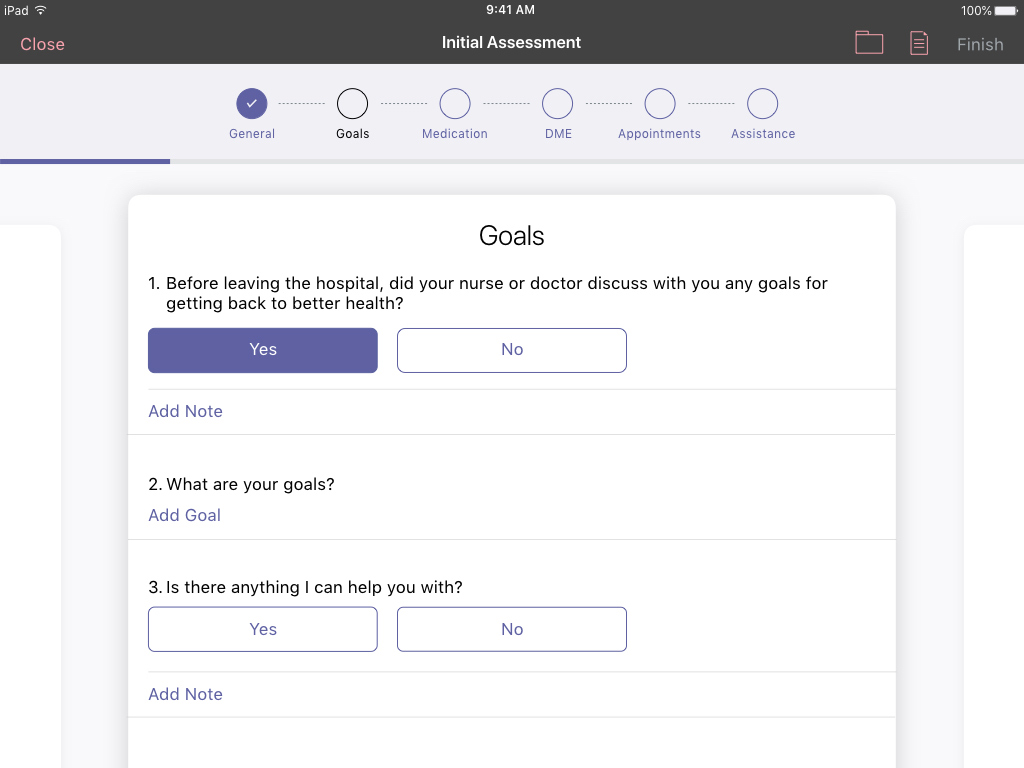
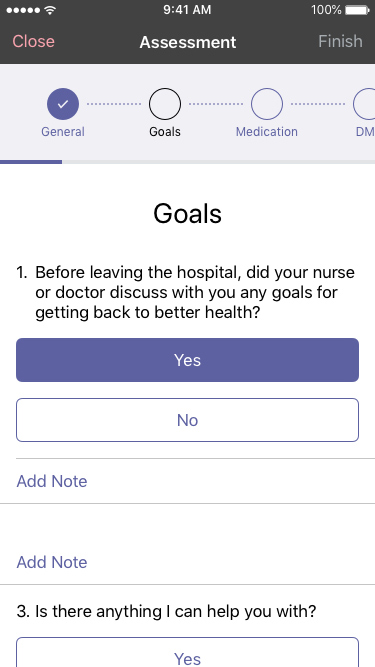
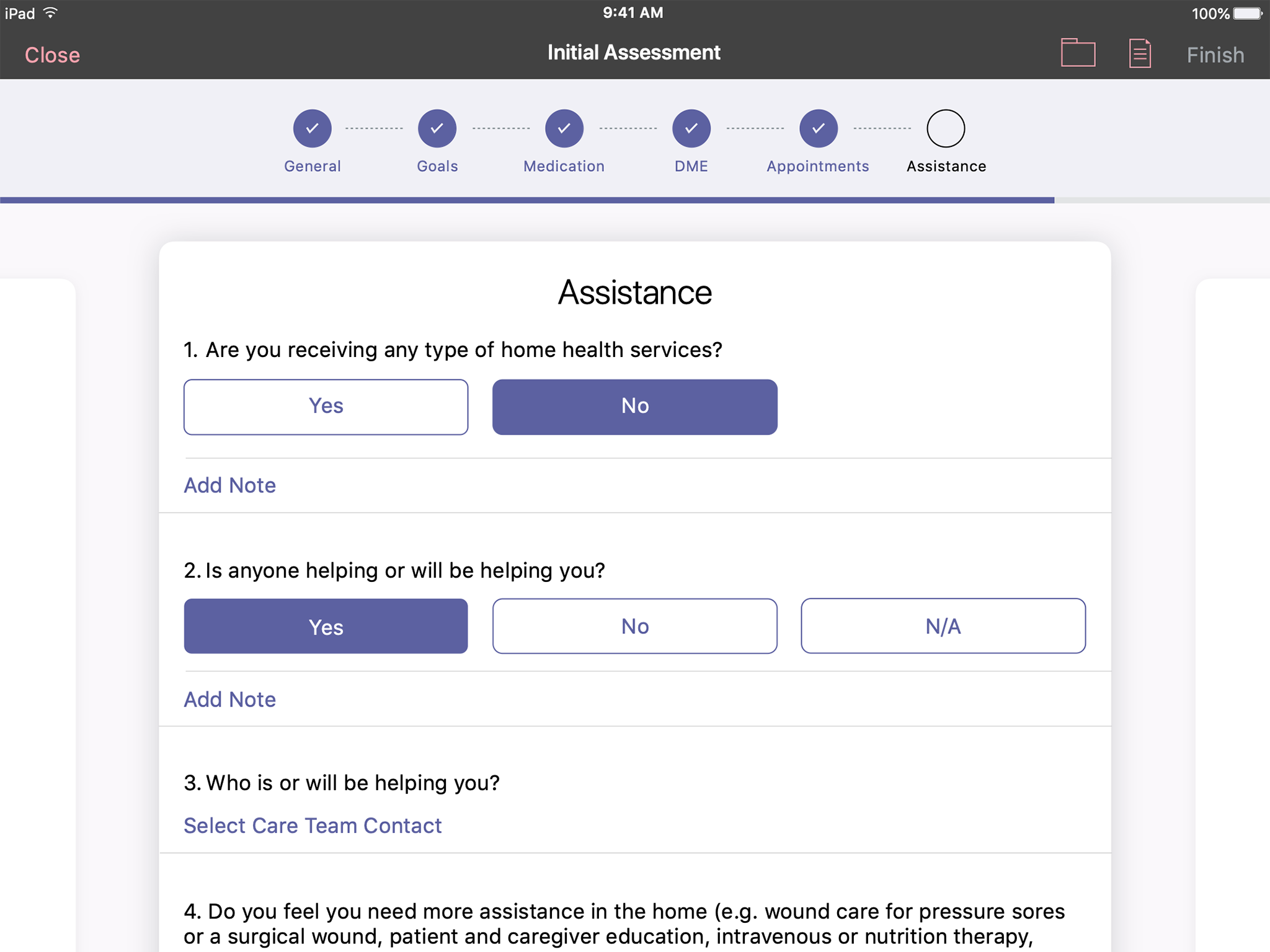
In order to stay engaged with the member, CM's took light notes while in the home but then had lengthy forms to fill out afterward. A structured, but low touch guided form allowed them to focus while in home and reduce post assessment work.